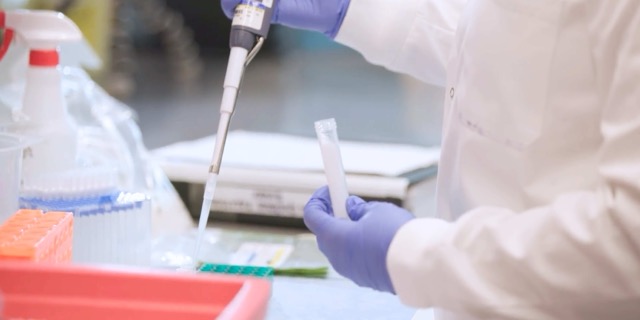
NEC Research Priorities
A collaborative project uniting patient-families and clinician-scientists to identify NEC research priorities, guiding critical funding and resources toward patient-centered solutions.
Micah
NEC Researchers
Let’s collaborate to advance the most urgent and impactful patient-centered research priorities.
Mapping NEC Research Priorities
When it comes to necrotizing enterocolitis (NEC), there are so many unanswered questions and limited resources. Our multidisciplinary team undertook a two-year project to identify research topics that matter most to patient-families and clinician-scientists. These priorities now guide funding and resources available for NEC research.
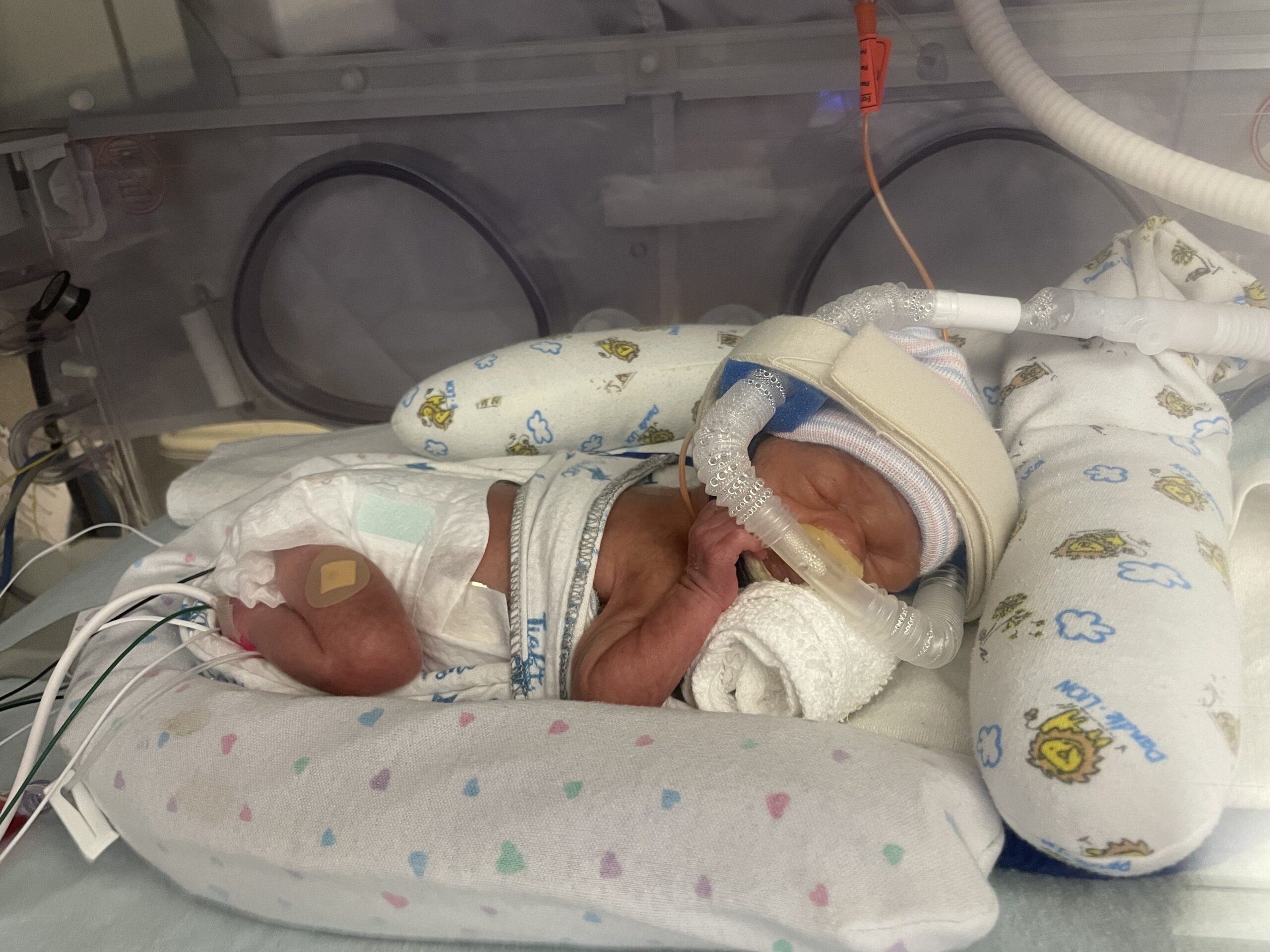
Identifying NEC Research Priorities
Over the course of this project, patient-families and clinician-scientists formed a team to identify the most pressing and important patient-centered NEC research questions.
The team first identified over 150 potential research opportunities, and collaboratively narrowed these to 20 prioritized topics, using the Delphi method. The full process will be formally published soon.
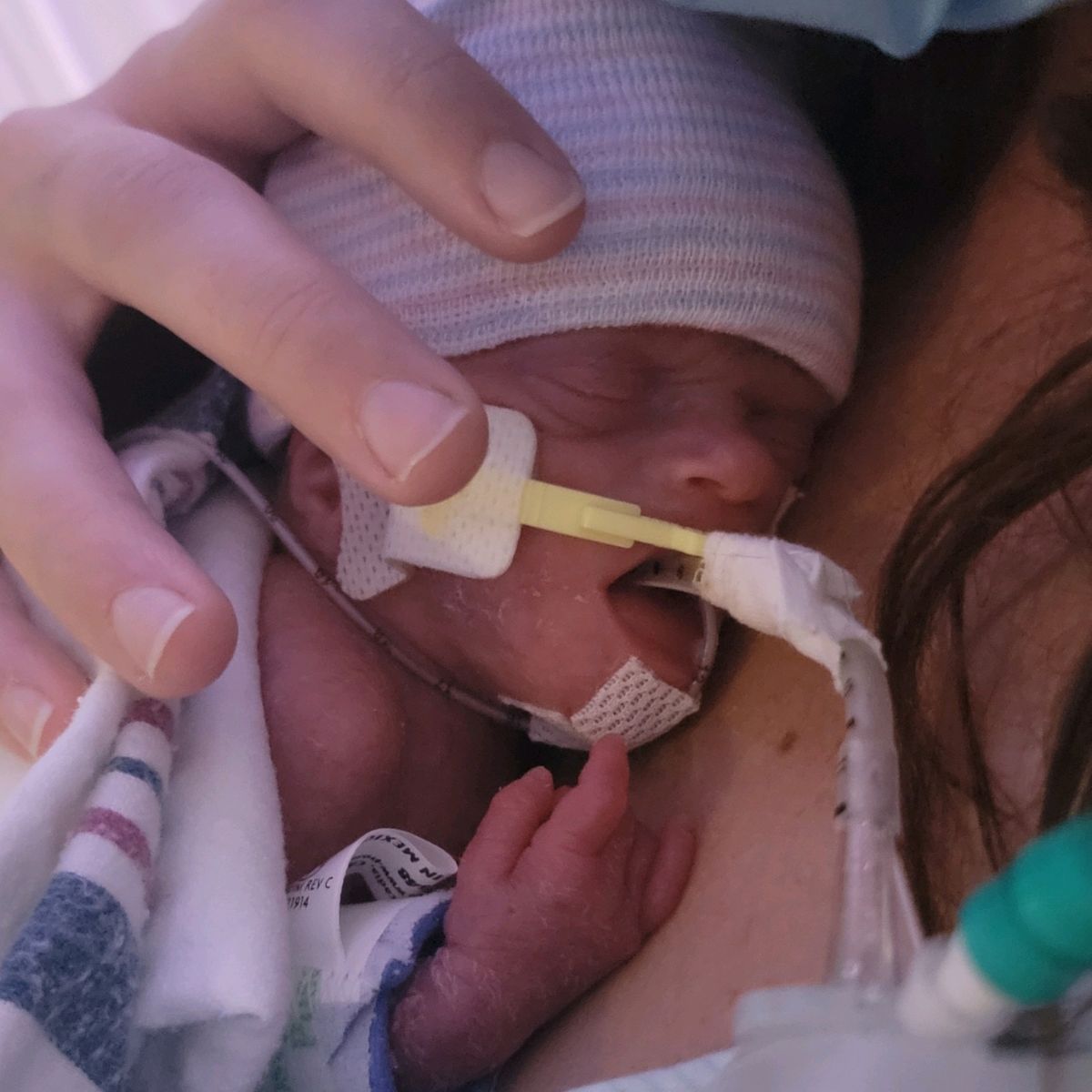
Patient-Centered Research Priorities
Research Priorities listed 1-20
- Development and use of medications or treatments to prevent NEC
- Optimizing the use of human milk and lactation support for prevention of NEC
- Tools, such as clinical scoring, biomarkers, or imaging, for the diagnosis of NEC
- Acute medical treatment and management of NEC, including novel treatments, biomarkers, imaging, antibiotic approaches, re-introduction of feeding, nursing care, treatment of pain, and avoiding brain injury
- Patient-family engagement, empowerment, and integration into the NICU care-team
- Long-term gastrointestinal outcomes, including short bowel and other non-neurodevelopmental health outcomes, from NEC that include quality-of-life measures
- Quality Improvement for NEC
- Identifying practices that increase NEC risk
- Long-term non-GI outcomes and fertility, and related quality of life measures
- Communication amongst the healthcare team and patient-families before and after NEC
- Proactive approaches to support patient-families with follow-up care and decisions, including developmental and intestinal failure care
- Chronic treatment and recovery of NEC, including subsequent surgeries, intestinal rehabilitation and transplant, as well as development of strategies to protect the liver and brain, and supporting transitions of care
- Educational approaches on NEC for patients and providers, before and after NEC
- Impact of nutritional composition and approaches including type, initiation, speed of advancement, standardized regimen, and feeding during transfusion
- Optimizing informed choice and shared decision making
- Fortification of human milk
- Initial surgical treatment of NEC
- Acute and long-term mental health of patient-families affected by NEC
- Financial and social-emotional burdens of NEC for patient-families, healthcare providers, hospitals, and society
- Disparities in NEC incidence and outcomes and inequity in decision-making and access to care and services
Check out our guide for other rare disease communities aiming to build a prioritized research agenda.
This project was made possible by an Engagement Award from the Patient-Centered Outcomes Research Institute (PCORI), and support from the Chan Zuckerberg Initiative.
Explore our community's research publications
Learn about the latest NEC research from publications written by the NEC Society’s Board, Council, Staff, and leading experts in the NEC community.